
Symptoms, Causes, Treatment Pathways & Professional Buyer’s Guide
Pelvic floor therapist guiding a patient through breathing and pelvic floor muscle assessment in a clinical therapy room.

Quick Answer
Yes, pelvic floor dysfunction can often improve. In some cases, symptoms may become minimal or disappear. But whether it truly “goes away” depends on the type of dysfunction, the cause, symptom severity, and whether the treatment matches the patient’s actual problem.
Pelvic floor dysfunction does not always mean weak pelvic floor muscles. Some patients have weak muscles, while others have overactive or tight pelvic floor muscles that cannot relax properly. This is why pelvic floor care should start with assessment, not with random Kegel exercises or device purchases.
What Is Pelvic Floor Dysfunction?
Pelvic floor dysfunction means the pelvic floor muscles and supporting tissues are not contracting, relaxing, or coordinating properly. The pelvic floor is a group of muscles, fascia, ligaments, and nerves located at the bottom of the pelvis.
The pelvic floor supports the bladder, uterus, rectum, and other pelvic organs. It also plays a role in bladder control, bowel control, sexual function, posture, and core stability.
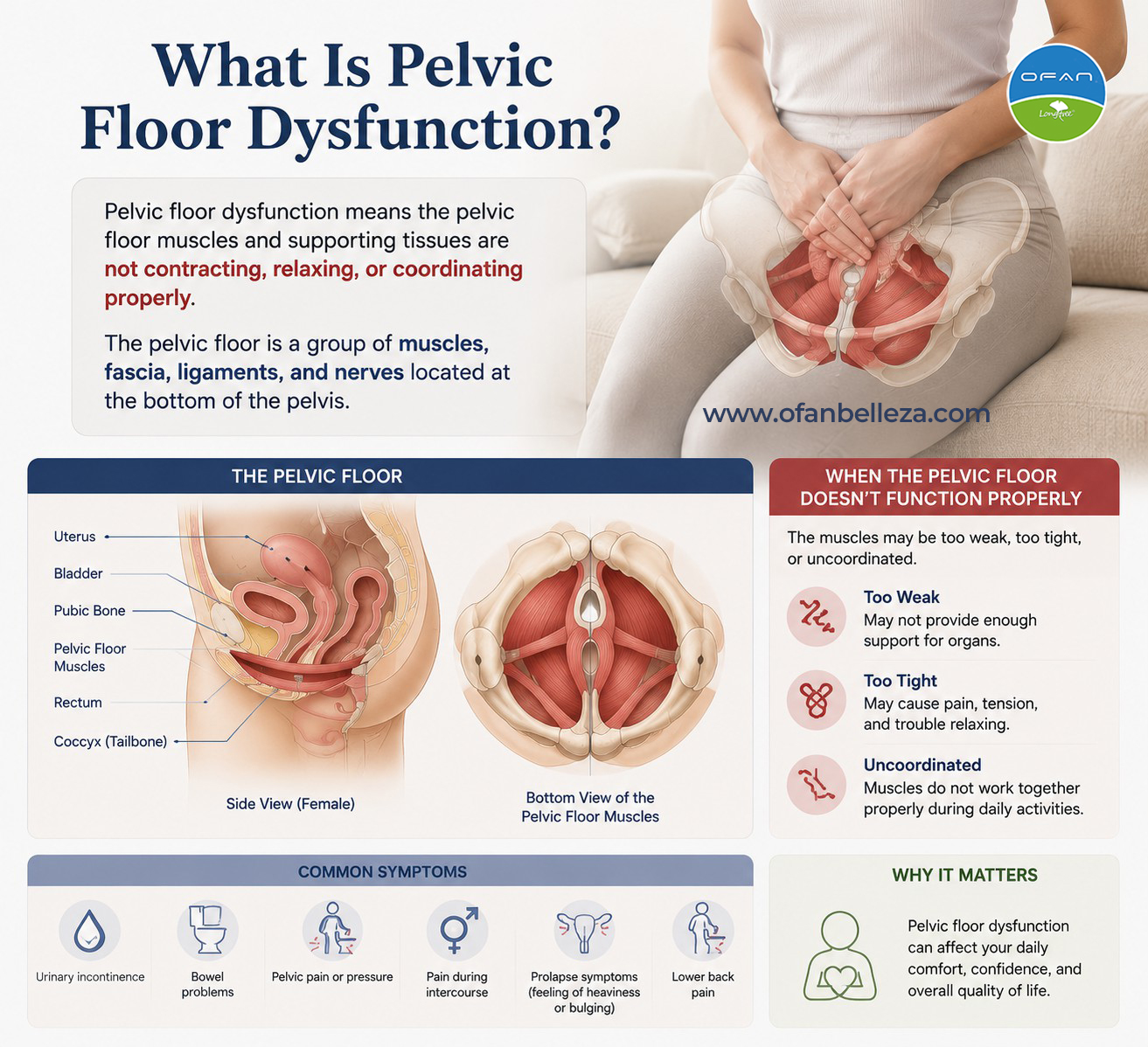
Pelvic floor dysfunction may involve:
- Weak pelvic floor muscles
- Overactive or tight pelvic floor muscles
- Poor coordination between contraction and relaxation
- Pelvic organ support problems
- Urinary symptoms, bowel symptoms, pelvic pain, or sexual dysfunction
Can Pelvic Floor Dysfunction Go Away on Its Own?
Mild pelvic floor symptoms may improve naturally, especially when they are temporary and linked to a clear trigger such as early postpartum recovery, short-term constipation, or a short period of heavy exercise.
However, symptoms that persist, return often, or affect daily life should not be ignored. If symptoms continue for weeks or months, professional assessment is usually more useful than waiting.
Symptoms That May Improve Naturally
- Mild postpartum urine leakage that gradually improves
- Occasional leakage only during high-impact exercise
- Temporary pelvic heaviness after constipation
- Mild symptoms that improve with rest, hydration, bowel regularity, and reduced load

Symptoms That Should Not Be Ignored
- Urine leakage during coughing, running, jumping, or lifting
- Ongoing urinary urgency or frequency
- Difficulty emptying the bladder or bowel
- A vaginal bulge or dragging sensation
- Pain during sex
- Pelvic, tailbone, rectal, or perineal pain
- Symptoms that worsen after Kegel exercises
- Postpartum symptoms that remain significant after several months

Is Pelvic Floor Dysfunction Curable?
Pelvic floor dysfunction can often be improved, and many people experience major symptom reduction. Some patients may become symptom-free. But “curable” depends on the diagnosis.
A patient with mild stress urinary incontinence may respond very well to supervised pelvic floor muscle training. A patient with advanced prolapse, nerve injury, chronic constipation, or long-term pelvic pain may need a longer-term treatment and management plan.
Recovery Potential by Problem Type
| Pelvic Floor Problem | Can It Improve? | Typical Treatment Direction |
|---|---|---|
| Mild stress urinary incontinence | Often yes | Supervised pelvic floor muscle training |
| Postpartum pelvic floor weakness | Often yes | Breathing, assessment, progressive strengthening |
| Overactive pelvic floor muscles | Often yes | Relaxation, manual therapy, coordination training |
| Mild to moderate prolapse | Symptoms may improve | PFMT, pessary, lifestyle changes |
| Advanced prolapse | Usually needs long-term management | Pessary or surgical consultation |
| Bowel coordination dysfunction | Often improves with therapy | Biofeedback, bowel retraining, physical therapy |
| Chronic pelvic pain | Variable | Multidisciplinary care, down-training, pain management |
Is Pelvic Floor Dysfunction Chronic?
Pelvic floor dysfunction can be short-term or chronic. It becomes more likely to persist when the underlying drivers are not addressed.
Common Long-Term Contributors
- Chronic constipation
- Chronic coughing
- Repeated heavy lifting
- Pregnancy-related tissue changes
- Menopause-related tissue changes
- Obesity or long-term high pelvic load
- Previous pelvic surgery
- Incorrect Kegel exercise habits
This is why pelvic floor care is not just about “squeezing harder.” A good treatment plan should look at breathing, bowel habits, bladder habits, pressure management, exercise load, pelvic pain, and tissue support.
Common Symptoms of Pelvic Floor Dysfunction
Pelvic floor dysfunction can affect the bladder, bowel, pelvic organs, sexual function, and pain system. Some people mainly have leakage. Others mainly feel pressure, pain, constipation, or difficulty relaxing.

Urinary Symptoms
- Leaking urine when coughing, sneezing, laughing, jumping, or lifting
- Sudden urge to urinate
- Frequent urination
- Night-time urination
- Difficulty starting urine flow
- Feeling unable to empty the bladder fully
Bowel Symptoms
- Constipation
- Straining during bowel movements
- Feeling blocked or unable to empty
- Needing to press around the vagina, perineum, or rectum to pass stool
- Faecal leakage
- Rectal pressure or discomfort
Pelvic Organ Prolapse Symptoms
- Vaginal heaviness or dragging
- Feeling a bulge in or near the vagina
- Pressure that worsens after standing
- Discomfort during exercise
- Difficulty inserting tampons or menstrual cups
- Bladder or bowel changes linked with pelvic pressure
Pain and Sexual Symptoms
- Pain with penetration
- Pelvic pain
- Tailbone pain
- Perineal pain
- Rectal pain
- Muscle spasm sensation
- Pain that worsens after Kegel exercises
Why Pelvic Floor Dysfunction Happens
Pelvic floor dysfunction is usually multifactorial. It is rarely caused by one single event. Tissue support, muscle control, nerve function, pressure management, lifestyle habits, and hormonal changes can all contribute.
Common Causes and Risk Factors
| Cause or Risk Factor | How It Can Affect the Pelvic Floor |
|---|---|
| Pregnancy | Increases load on the pelvic floor and abdominal pressure system |
| Vaginal childbirth | May stretch muscles, fascia, and nerves |
| Assisted delivery | May increase pelvic floor strain |
| Chronic constipation | Repeated straining increases downward pressure |
| Chronic cough | Repeated pressure spikes stress pelvic support |
| Obesity | Adds long-term load to pelvic tissues |
| Menopause | Can affect tissue elasticity and vaginal comfort |
| Pelvic surgery | May alter support structures or nerve function |
| High-impact sports | Can overload the pelvic floor if coordination is poor |
| Overactive muscles | Can cause pain, urgency, and difficulty relaxing |
Treatment Pathway: What Actually Helps?
The right treatment depends on the type of pelvic floor dysfunction. A person with weak pelvic floor muscles needs a different plan from someone whose pelvic floor is tight, painful, or unable to relax.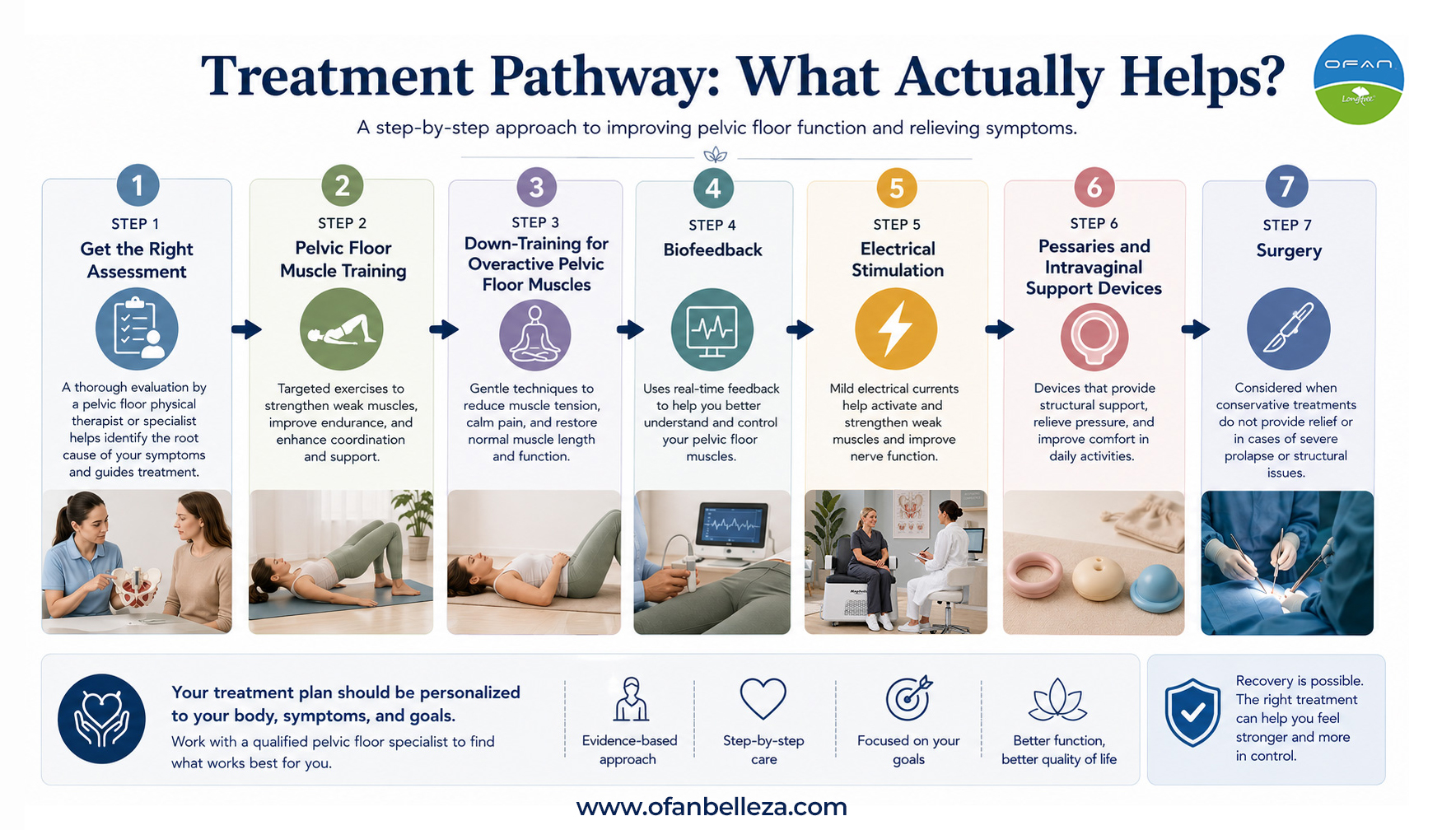
Step 1: Get the Right Assessment
A pelvic floor assessment may include symptom history, pregnancy and birth history, bladder and bowel habits, pain triggers, breathing and pressure management, pelvic floor contraction and relaxation ability, prolapse screening, and review of exercise or lifting habits.
Step 2: Pelvic Floor Muscle Training
Pelvic floor muscle training is often used for stress urinary incontinence, mixed urinary incontinence, postpartum weakness, and some prolapse symptoms. However, effective training is not just repeated squeezing.
A good pelvic floor training program may include:
- Correct muscle identification
- Full relaxation between contractions
- Strength and endurance training
- Quick contractions for cough, sneeze, or impact control
- Breathing coordination
- Functional training during lifting, running, or jumping
Step 3: Down-Training for Overactive Pelvic Floor Muscles
Not every patient needs strengthening first. Some need to learn how to relax. Down-training may be especially important for patients with pelvic pain, painful sex, constipation with outlet difficulty, urinary urgency, or symptoms that worsen after Kegel exercises.
Down-training may include:
- Diaphragmatic breathing
- Pelvic floor relaxation
- Hip and pelvic mobility work
- Manual therapy
- Nervous system calming strategies
- Bowel retraining
- Gradual return to exercise
Step 4: Biofeedback
Biofeedback can help patients understand whether they are contracting or relaxing the pelvic floor correctly. It is especially useful when a patient cannot feel the muscles clearly or struggles with coordination.
Biofeedback is not a magic shortcut. Its value is in teaching awareness, improving technique, and supporting a structured therapy plan.
Step 5: Electrical Stimulation
Electrical stimulation may be considered when the pelvic floor muscles are very weak or when the patient cannot voluntarily contract them effectively. It should be selected carefully because treatment intensity, frequency, session time, contraindications, hygiene, and comfort all matter.
Step 6: Pessaries and Intravaginal Support Devices
Pessaries can be useful for symptomatic pelvic organ prolapse. They are placed inside the vagina to support pelvic organs. A pessary should be fitted and reviewed by a qualified healthcare professional.
Step 7: Surgery
Surgery may be considered for advanced pelvic organ prolapse or severe urinary incontinence when conservative treatment is not enough. The decision should consider symptom severity, age, tissue health, sexual function, future pregnancy plans, surgical risks, recurrence risk, and patient preference.
Professional Buyer’s Guide: How to Choose Pelvic Floor Products
Pelvic floor products should not be purchased only because they look modern, connect to an app, or promise “tightening.” For clinics, distributors, pelvic health brands, postpartum centers, and rehabilitation providers, the best purchasing decisions are based on clinical fit, safety, usability, compliance, evidence, and after-sales support.
Main Product Categories
| Product Category | Best Use Case | Buyer’s Notes |
|---|---|---|
| Biofeedback devices | Muscle awareness, assessment, guided training | Check sensor accuracy, software reports, patient usability |
| Electrical stimulation devices | Very weak muscles, poor voluntary contraction | Check parameter control, contraindication warnings, safety documentation |
| Pelvic floor trainers | Home training and maintenance | Check app quality, privacy policy, cleaning instructions |
| Vaginal probes | Clinical assessment or device-based training | Check material, size options, sterilization or single-use policy |
| Vaginal cones or weights | Progressive strengthening in selected users | Not ideal for pain, overactivity, or unclear diagnosis |
| Pessaries | Pelvic organ prolapse support | Requires fitting, sizing, follow-up, and patient education |
| Education kits | Patient education and clinic demonstrations | Useful for anatomy explanation and compliance |
| Software systems | Rehab center workflow and patient tracking | Look for reports, progress tracking, and data protection |
Partner with OFAN for Pelvic Floor Therapy Equipment
OFAN has been dedicated to pelvic floor therapy device design and manufacturing since 2008. We provide professional pelvic floor therapy equipment for women’s health clinics, postpartum recovery centers, rehabilitation providers, aesthetic medicine businesses, and medical device distributors.
With OEM/ODM support, OFAN can help partners develop private-label pelvic floor therapy devices, customize appearance and functions, and build product solutions that fit local market needs.
Need help choosing the right pelvic floor therapy device? Contact OFAN today👉Get Quote Nowto discuss your project, product requirements, and cooperation plan.
OFAN Clinic Pelvic Floor Therapy Machine
👉Contact OFAN for OEM/ODM Pelvic Floor Therapy Device Solutions
👉Click to View: Pelvic Floor Therapy Machine
Procurement Checklist
- Is the product intended for professional or home use?
- Does it have appropriate regulatory clearance for the target market?
- Are indications and contraindications clearly stated?
- Is the device suitable for weak muscles, tight muscles, prolapse, pain, or incontinence?
- Does it support both contraction and relaxation training?
- Are probes or intravaginal parts made from body-safe, medical-grade materials?
- Are cleaning, disinfection, or replacement instructions clear?
- Can the software generate patient progress reports?
- Is patient data protected and exportable?
- Are training materials available for clinicians and patients?
- Are consumables easy to reorder?
- Does the supplier offer warranty, repair, calibration, and clinical onboarding?
Deep Comparison: Biofeedback vs Electrical Stimulation vs Pessary vs Surgery
Different pelvic floor solutions are not interchangeable. A biofeedback system, an electrical stimulation device, a pessary, and surgery solve different problems. Good clinical decision-making starts with the patient’s symptom pattern, not with the product category.
| Option | Best For | Strengths | Limitations |
|---|---|---|---|
| Pelvic floor physical therapy | Most pelvic floor dysfunction types | Individualized, diagnosis-driven, adaptable | Requires appointments and consistency |
| Biofeedback | Poor muscle awareness or coordination | Makes muscle activity visible | Does not replace clinical judgment |
| Electrical stimulation | Very weak pelvic floor contraction | Can help activate muscles | Not suitable for everyone |
| Vaginal cones | Selected strengthening cases | Simple progressive resistance | Poor choice for pain or overactive muscles |
| Pessary | Symptomatic prolapse | Non-surgical support | Needs fitting and follow-up |
| Surgery | Severe prolapse or refractory incontinence | Can address structural problems | Risks, recovery time, recurrence possible |
Biofeedback vs Electrical Stimulation
| Feature | Biofeedback | Electrical Stimulation |
|---|---|---|
| Main role | Shows muscle activity | Stimulates muscle activation |
| Patient participation | Active | More passive |
| Best suited for | Learning technique and coordination | Very weak or poorly activated muscles |
| Useful for relaxation? | Yes, depending on system | Less commonly the main use |
| Main risk | Over-reliance on screen numbers | Discomfort, incorrect use, contraindications |
| Best setting | Clinic or guided home program | Professional guidance recommended |
Home Device vs Clinic Treatment
| Feature | Home Device | Clinic Treatment |
|---|---|---|
| Convenience | High | Lower |
| Personalization | Limited | High |
| Assessment quality | User-dependent | Professional |
| Best for | Maintenance, mild cases, guided programs | Pain, prolapse, complex symptoms, poor technique |
| Main limitation | May be misused | Requires time and cost investment |
For Distributors and Medical Device Buyers
Prioritize regulatory readiness, product documentation, and training resources. Pelvic floor products are sensitive because they involve intimate use, health data, and clinical claims.
- Market-specific compliance
- Labeling and instructions for use
- Contraindication documentation
- Clinical training materials
- Complaint handling process
- Replacement parts and consumables
- Software privacy and cybersecurity policies
For Patients Choosing a Home Device
Do not buy based only on social media claims. A home pelvic floor device may be useful if a healthcare professional confirms that it fits your symptoms and you understand how to use it safely.
Avoid self-selecting a device if you have:
- Pelvic pain
- Pain during sex
- Vaginal bleeding
- Active infection
- Pregnancy-related concerns
- Recent pelvic surgery
- Severe prolapse
- Symptoms that worsen with Kegel exercises
When to See a Doctor or Pelvic Floor Therapist
Seek professional evaluation if you have leakage that affects daily life, pelvic heaviness, a vaginal bulge, pain during sex, chronic pelvic pain, difficulty urinating, difficulty emptying the bowel, recurrent urinary tract symptoms, faecal leakage, symptoms after childbirth that do not improve, symptoms after pelvic surgery, or Kegels that make symptoms worse.
Pelvic floor dysfunction is common, but it should not be dismissed as “normal.” Many symptoms can be managed better when they are assessed early and treated according to the real cause.
FAQ
What is pelvic floor dysfunction?
Pelvic floor dysfunction means the pelvic floor muscles and supporting tissues are not working properly. They may be weak, too tight, painful, poorly coordinated, or unable to support the pelvic organs effectively.
Can pelvic floor dysfunction go away?
Yes, pelvic floor dysfunction can improve significantly, and some people become symptom-free. The result depends on the cause, severity, and whether treatment matches the type of dysfunction.
Can pelvic floor dysfunction be fixed?
Many cases can be managed or corrected with pelvic floor physical therapy, supervised pelvic floor muscle training, lifestyle changes, biofeedback, electrical stimulation, pessaries, or surgery when needed.
Will pelvic floor dysfunction go away without treatment?
Mild and temporary symptoms may improve without formal treatment. Persistent leakage, pain, prolapse symptoms, or bowel and bladder difficulty usually need professional assessment.
Is pelvic floor dysfunction chronic?
It can become chronic if the underlying causes are not addressed. Chronic constipation, coughing, poor pressure management, untreated prolapse, or incorrect exercises can keep symptoms going.
Is the pelvic floor curable?
The pelvic floor itself is not a disease. But pelvic floor weakness, tension, and coordination problems can often be improved. Some structural problems may need long-term management or medical treatment.
Final Takeaway
Pelvic floor dysfunction can often improve, but the key is choosing the right path. Weak muscles may need strengthening. Tight muscles may need relaxation. Coordination problems may need biofeedback. Prolapse may need pelvic floor training, a pessary, or surgical consultation.
For patients, the first step is not buying the newest device. It is understanding the type of dysfunction. For clinics and buyers, the best pelvic floor products are not the ones with the most features. They are the ones that fit real clinical workflows, protect patient safety, support accurate assessment, and help users follow a structured treatment plan.
Information
Author Bio
This article was written by a pelvic health content editor specializing in women’s health education, postpartum recovery, pelvic rehabilitation products, and non-surgical pelvic floor care pathways.
Medical Review
Recommended for review by an OB-GYN, urogynecologist, or pelvic floor physical therapist before publication, especially for sections related to diagnosis, contraindications, device use, prolapse care, and treatment pathways.
References
- NICE: Pelvic floor dysfunction: prevention and non-surgical management
- ACOG: Pelvic Support Problems
- Mayo Clinic Health System: Pelvic floor physical therapy benefits
- Cochrane: Pelvic floor muscle training for urinary incontinence in women
Disclaimer
This article is for health education and product selection reference only. It does not replace medical diagnosis, professional evaluation, or treatment from a licensed healthcare provider. People with pain, bleeding, significant prolapse, urinary retention, bowel emptying difficulty, severe postpartum symptoms, or symptoms after pelvic surgery should seek medical care.































